It has been many months since completing my treatment for rectal cancer. My tumour is gone. I’m clear. I’m back. I have felt compelled to write about the experience yet lacked the motivation to do so.
At the same time I am stuck between two approaches to this story. I could compress it into a succinct, digestible feature or I could drag out the entire history in raw detail. The editor in me is screaming to throw the sandbags out of the basket and keep it tight but I wonder if some poor soul out there might stumble upon my crude journalling at a difficult time and take heart from all the nuanced, mundane reality of what happened.
Obviously I’m running with Option B: bore them with trivialities. If you just want the juice, skip straight to the last section.
Part 1: Crash
I wrote an earlier piece shortly after I was diagnosed, during the last gasps for air before the dive into treatment. Now I want to round off this episode in my life with some thoughts. And as I struggle to extract meaning from what happened, I feel compelled to start by revisiting the day of my diagnosis: Thursday 16 February, 2017.
At the time, there had been blood in my stools for a year, and in recent months I had developed a frequent sense of urgency to rush to the loo. Nothing else. No loss of weight, exhaustion, nausea or other alarm bells. My GP, who had examined me within a week of the symptoms first appearing, had concluded that it was probably just haemorrhoids but had referred me for a colonoscopy anyway. After that I just waited for the appointment. For months.
After continued nagging from my loved ones, I finally paid for a private consultation, and a week later I also paid for a colonoscopy. Did going private save my life? I don’t know. I would find out later that the 45-minute colonoscopy appointment for which I had been referred on the NHS took over a year to finally come through, long after I had been diagnosed privately and undergone treatment. By that time my tumour could have got out of control, metastasised, killed me. Maybe. It’s impossible to know but it’s still sad.
The consultant was friendly. He took an interest in my job and asked if I’d met a woman over here. He asked if I had any kids from my earlier marriage. He pushed a latex-gloved finger into my back passage, then looked inside me through a plastic probe before going in with the finger for a second time, to make sure. Once I was back on my feet he said, quickly and simply, it was bad news. He told me that the haemorrhoids ‘had been a red herring’, that he could feel a lesion. He called it ‘lesion’ only the first time. That didn’t sound too bad to me, like a scar.
The consultant explained that scans were needed to determine the object’s nature and to look for anything else in me. If it was cancerous, he said, I was well placed as a healthy man in his thirties. ‘You’ll be a survivor’, he said, ‘I’m sure of that’. There was real sadness in his tone, he was sorry that it should happen to me. I told him it was OK, I told him not to be sorry.
Before he’d broken much of the news, the consultant asked me at least one more time if I had any kids. I guess he wanted to know what the effects of the situation would be. At the time I thought it was just friendly conversation. When I search online for his biography the next day, one piece of text really stood out: ‘Married to Angela. Triplets Conor, Cameron, Anna – born 2002’. I pictured three fourteen year-olds running about the house, all similar yet individual in different ways.
I walked out of the hospital and into the Belfast winter. It was one of those days when even the clouds can’t be bothered, they just loiter at street level and soak everything that dares to step outside. The air was cool but not unusually so for that time of year. There was a scent around that I couldn’t quite place, smoky but without the homely sweetness of Ireland’s ubiquitous peat fires. Although I was walking in my usual vigorous march, I couldn’t get warm. A chill sat on my lower back and wouldn’t leave. I knew what it was: the comedown from mild shock.
As I marched through the drizzle I pressed the shutter on my mental camera, assigning the view ahead to permanent memory, filed under the category of those rare days that really mean something.
Maeve got home from work a few minutes behind me. She asked me about my appointment as soon as she entered the living room, before she had sat down and got comfortable.
‘It’s not a haemorrhoid’, I said, ‘it’s a tumour’.
‘You’re joking’, she replied instinctively. I wasn’t expecting that.
‘No, he found something up there’, I replied.
I tried to tell her the news in the most coldly factual way I could, theatrics weren’t going to help. But it was Maeve who did the better job of sucking the drama out of my words. She gently hugged my arm and led me to the sofa so we could sit right against each other. As we talked the situation through, Maeve kept catching me out for making statements about things I couldn’t yet know. She confidently explained that the thoughts of cancer were inevitably where I might go, when in reality cancer was the other side of multiple ifs.
I wish I had been slightly calmer when I told Maeve. I let the story overpower me. I told her that I was sorry for letting her and my loved ones down by not following their pleas to get examined sooner, and as I said those words my eyes started to water. Hers replied in kind, but she fought them back with a smile, through which she gently ordered me not to cry.
Minutes later we were making dinner together and nothing was different about the scene from any other Thursday. We elected to go to the cinema as a distraction but even that was a normal weekday activity anyway.
Sidenote: Journal extract, 17 Mar 2017:
Adenocarcinoma, now I know what species Tony* is. Adenocarcinoma, now the word floats around in my head. I play with the emphasis, shifting it from the second to the first syllable and back again: ‘ADDeno, adEEno’. ‘ADDeno, adEEno’.
My oncologist told me that adenocarcinoma is the ‘normal bowel cancer’. OK, is that good? Should I prefer that to something less normal? The only meaning I have derived from that statement is that normal probably means common and common is likely to be well studied. Therefore I might be able to find more helpful literature on how to handle my enterological house-guest than on a rarer alternative. ‘House guest?’ Well, I suppose ‘squatter’ would be more appropriate.
*Tony is the name we gave to my tumour. Wondering why? If you don’t already know the story, don’t ask. Let’s just say I named it after someone who deserved it.
Part 2: Patch
I was prescribed a combined course of chemo- and radiotherapy for five weeks, to commence immediately and run into May. Burn the bastard out.
The chemo was simple, just take a fistful of pills every day. You might get nauseous, your skin might turn red, your bodily fluids could be toxic to everyone around you, oh the list goes on. My favourite side-effect, the one that made me laugh in front of my oncologist, was that chemotherapy can be carcinogenic.
Lol. I think that’s what you call irony.
For the radiotherapy, I had to attend the hospital for a brief session each day. I requested the earliest slot possible so I could get in and away quickly. I could walk to the hospital for eight a.m., get zapped by high-energy X-rays and still be in the office fifteen minutes early.
I was asked to arrive half an hour early each day, to prep. This simply involved drinking enough water to ensure my bladder was full before the session. With my long-establish habit of drinking plenty of water each day – something I couldn’t advocate enough but won’t digress into now – I didn’t need to attend the prep period. But I went anyway because some creative time had been forced into my day. For most of the five-week period, I sat in the waiting area, taking online lessons in software coding, while my fellows stared into space or the pages of trashy magazines. Time lost for them, gained for me.

The treatment suite was a squarish room about six metres to a side. Consuming the room’s space was a huge machine – a Varian TrueBeam ‘high-precision radiotherapy treatment system’. It consisted of a flat, black carbon-fibre bed at one end, and the main delivery system at the other, which was off-white, about three metres tall and wide, with four curving heads that extended out from it and peered down on the bed. It had a futuristic, spacey, alien quality, like some robot bird-of-prey crouching over its victim
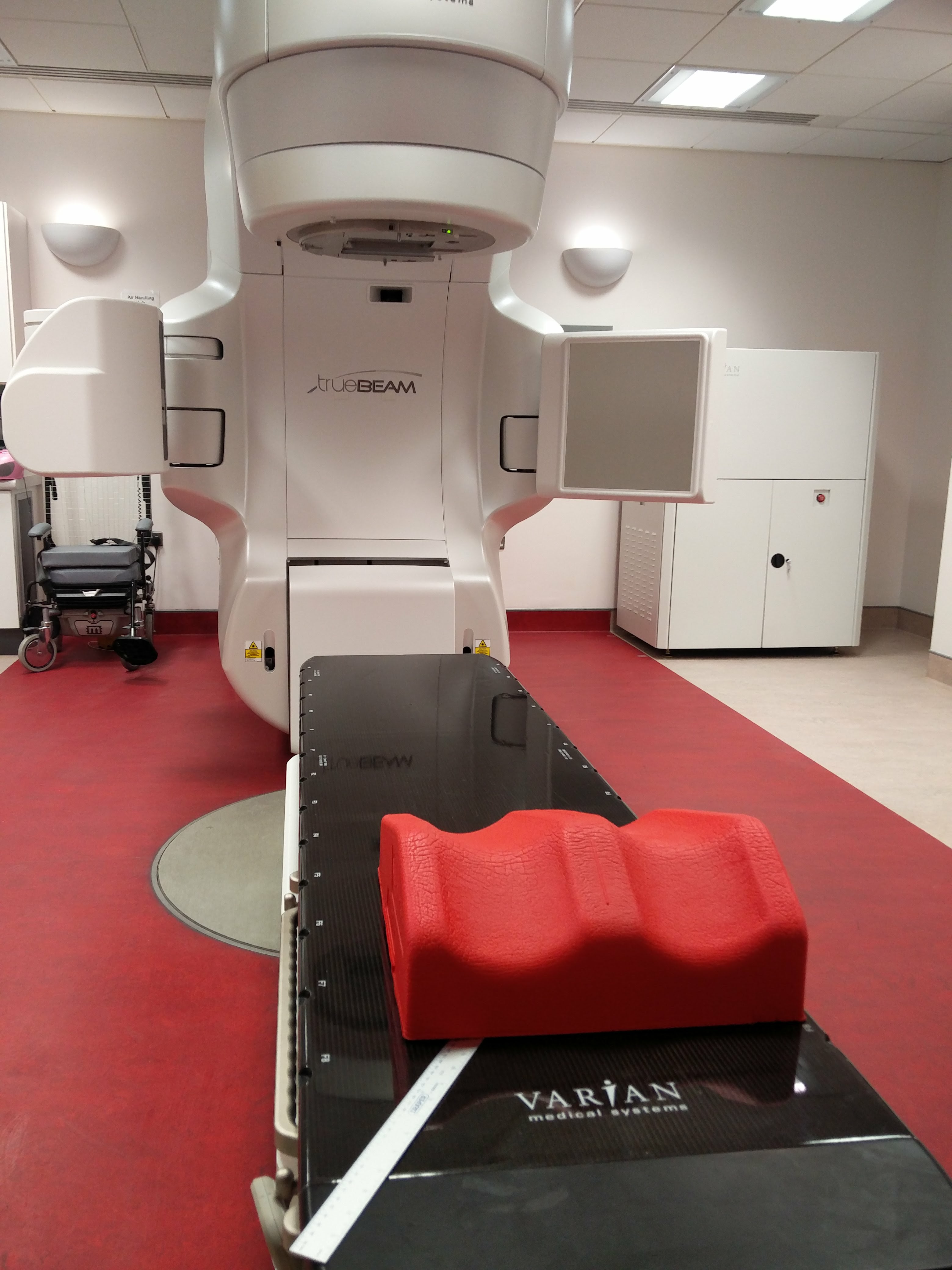
I soon learned the drill. I took my shoes and trousers off and climbed on to the cold, hard bed, lying face-down with my head resting to one side on my arms, which were folded over a pillow with a plastic case. I lifted my feet automatically as the nurses placed a support cushion under them to keep them raised and still. Then I lifted my pelvis so they had room to pull my boxers down and expose my bum to the machine that was hunched expectantly over me. Once I was settled, the bed was moved up and forward to a high position between the machine’s multiple heads.
I immediately closed my eyes and slowed my breathing, half listening to the nurses working around me. They would lift and twist a leg slightly, or push a bum cheek so it settled back a few millimetres to one side, trying to align my body to the lasers pointed at it. As my mind began to unwind in those few minutes of involuntary stillness, the nurses quietly called out their measurements, each double checking the others’ work.
‘I need a half drop on my side, how’s your side?’
‘Fine, you can take it.’
‘Breathing through.’
‘Inf, six point five.’
‘Post, eleven.’
‘Eight point three, ninety-three point five.’
‘Perfect.’
Then they would swiftly leave the room, with one of them calling back to me – something along the lines of, ‘OK Ben, we’ll see you in a minute.’
I would mumble reassuringly into the flesh of my forearm as I drifted into a stupor with the machine whirring softly around my head. About five minutes later I would hear footsteps returning to the room, accompanied by voices. The bed would start to retreat down and back. I would open my eyes then and, through the bleariness of half sleep, see the heads of the machine rotating back to their own original position. Around me, red and green laser beams criss-crossed my body and flashed across my face. It created a scene like something out of a sci-fi movie, as if I was floating backwards along the corridor of a spaceship, spinning slowly in the absence of gravity.
For a darkly serious process such as cancer treatment, the radiotherapy was, at least for me, a bit of fun each morning. By the time I left the therapy suite I had completed a decent morning ritual of learning and meditation, ready for the working day. I would have paid for such a productive routine. Oh, except for the radiation scorching my internal organs I guess. One side-effect of intensive X-ray bombardment is, yeh, you guessed it: cancer.

Part 3: Reboot
When I arrived on the ward in July, for the first and biggest of my two surgical procedures, I was led to a mechanised hospital bed in one of six identical bays. Each bay occupied an area just bigger than its bed, defined by a blue curtain that was almost permanently open.
I raised the head of the articulated mattress on my bed so I could sit up and immediately, somehow, I became a patient. I was fully clothed and in good health but the surrounding environment quickly overpowered me. The utilitarian interior, and all those sick-looking, older, sagging people, made me feel helpless and slow. I became one of them.
Some time the following evening I hauled my heavy eyelids up and found myself somewhere unfamiliar. I was reclined, head propped up on a pillow, looking into a dimly lit room. After a few seconds my eyes automatically rolled shut. After an unknowable time I opened them again, then closed them. I think this happened two or three times before I fully awoke. I’m not sure, it’s hard to remember. But when it finally happened, I think I told myself, ‘hey, you’ve just had surgery, you’re in the recovery ward’.
Then, ‘you did it’.
My body felt like it was hanging in some barely attached existence beneath my head, as if I was submerged to my neck in a pool of thick, warm liquid. I don’t know if I had the good sense to avoid making any sudden moves or if the stupor of anaesthetic and exhaustion had already induced me to stillness.
I don’t know how long I was there.
The girls – my wife and our dear friend – were waiting for me. I don’t know for how long.
I sucked a lemon-flavoured swabbing stick and wet my lips with it. It tasted like battery acid but the touch of moisture and hydration were welcome. That was the first small step on the slow haul back.
Back on the ward, each of the next ten days were similar, not just in terms of activity but also in my state of being. Every day virtually the same, staring at the same view. It was only the cast of characters around me that changed, as medical staff switched shifts, and discharged patients were replaced with new ones. Every day like the other, except Saturday. Saturday was rough.
A nurse told me that Day Three is a classic post-surgery low point. I had been taking my anaesthetic via an epidural in my back but they removed it at that point and moved me over to a course of long- and short-acting opiate pills, plus paracetamol via a drip in my arm. Something about the transition from one drug to another set off a reaction from my body.
It started with a rising sense of hot pain coming directly from the foot-long surgical incision running vertically across my belly. I could feel the wound for the first time, it was really there. And it burned. It was a rasping sting, like tearing off a plaster. It would have been bearable for a few minutes but it persisted for two, three, maybe four hours. I breathed through it, watching a TV show to distract myself, until the pain finally began to subside. It was replaced with a far worse sensation of nausea that rolled in and out in slow waves, making me feel hot then cold; tired then restless; drowsy then anxious. When I closed my eyes to escape I hallucinated, falling through star-fields and complex structures that spun in blackness in front of me, making me dizzy with vertigo.
My girls were with me on that day too. They watched me go under. It was hard for them. I would haul my eyelids open, sigh noisily and see them cry. ‘It’s OK’, I would croak, ‘I’m OK’. Then I would drift back into the abyss. It was a rough ride but it felt like it had a place in the process – like something I was due, like a really nasty hangover. I knew the ride would end eventually.
At some point I fell asleep. I woke at a normal time the next morning feeling rested and free of pain. Soon after that I spotted the long-acting opiate pill resting in the poo tube that emerged from my abdomen. It had passed through my body untouched. After that I refused any painkillers stronger than paracetamol having learned by accident that I could get through without them.
I spent all day in bed, broken by a few visits to the toilet just outside the ward. Walking there, I stooped and dragged my feet, moving slowly to avoid jarring myself. My voice was strained and weak. My T-shirt had blood stains on it and a clear, shit-filled incontinence bag hung from the side of my belly. My life felt very far away.
With each day I gained a little more energy and mobility. One by one the NHS staff pulled tubes from me. Tubes that had been wormed into my arms, my belly, my back and my penis, some to remove fluid, some to add it. After a week I was just bored and grumpy, waiting for my wound to settle from a mild infection before I could leave.
I was discharged after eleven days in hospital, which was normal for the procedure I had had: a ‘low anterior resection’. Eleven days is not a long time but it felt like it, like months, like an entire chapter in my life. By the time I left, I was shuffling about with confidence and the gaping slices through my abdomen were clearly starting to close. I had been powered down, rewired then switched on again. The care I had received, from many kind and skilful members of our free health service, had been to supervise a deep reboot of this faulty human.
Part 4: Run
That’s basically it. Although my treatment would not conclude for another ten months, my journal is almost empty during that time. I don’t have much to tell. But then, I think there’s something significant in the silence.
The biopsy on the section of colon and rectum that my surgeon removed showed a tiny trace of cancer on a lymph node that had been excised with the rest of the tissue. It was enough to validate a second round of chemotherapy. This time it was to be five months of pill popping. The stoma bag attached to my belly would have to remain at least until I was through that period of swallowing toxic medicine, due to the immunosuppressive effects of chemo.
The pill routine went thus: fourteen days of taking two rounds of Capecitabine pills a day, then seven days off before repeating the process. Seven rounds of that procedure took me up to 1 February the following year. During that time, and up until my final, second surgery in early May, I was pooing into a bag that hung from my belly, under my clothes.
When I finally emerged from the swamp of medicalisation, dropping my last round of pills over breakfast in February 2018, I ran the numbers: since diagnosis a year earlier I had consumed 713 Capecitabine pills, amounting to a whopping 304.7 grams. Add to that an estimated 677 anti-diarrhoea pills. That’s… well of course I kept all the packets to count them.
I’m lucky I guess. ‘Chemo’ carries such a dark weight of meaning. It can wipe people out. But the effects vary across people and circumstances, and there are many different forms and doses. I had a relatively gentle version. Added to that, I was young and fit compared to your average cancer victim. So I barely suffered. No nausea, no tiredness, no hair loss (not that I had any hair anyway!). And shitting into a bag became normal almost instantly.
Finally, on Wednesday 2 May 2018, I went back to the same hospital I had been in almost a year earlier, to complete the process. I was to go under the knife of the same surgeon as before. In fact he was the same person who had diagnosed me in the first place, once more directing my life with a flick of his expert fingers. This final surgical procedure was an ileostomy reversal. In the original surgery to remove part of my colon and rectum, my surgeon had also pulled a loop of my small intestine (ileum) out through the skin of my belly. It acted as a kind of bypass so my poo would head straight out through the hole – the stoma – and avoid infecting the damaged guts further down.
My stoma was weird. It had an impossibly bright pink colour, glimmering in the constant supply of moisture that coated it. It looked like a dog’s penis, or Gonzo’s nose, or something. And it moved – recoiling, changing direction then probing out again – with unnerving autonomy. Occasionally it ejected some poo. I couldn’t feel it and I had no control over it. It was like living with a harmless alien parasite.
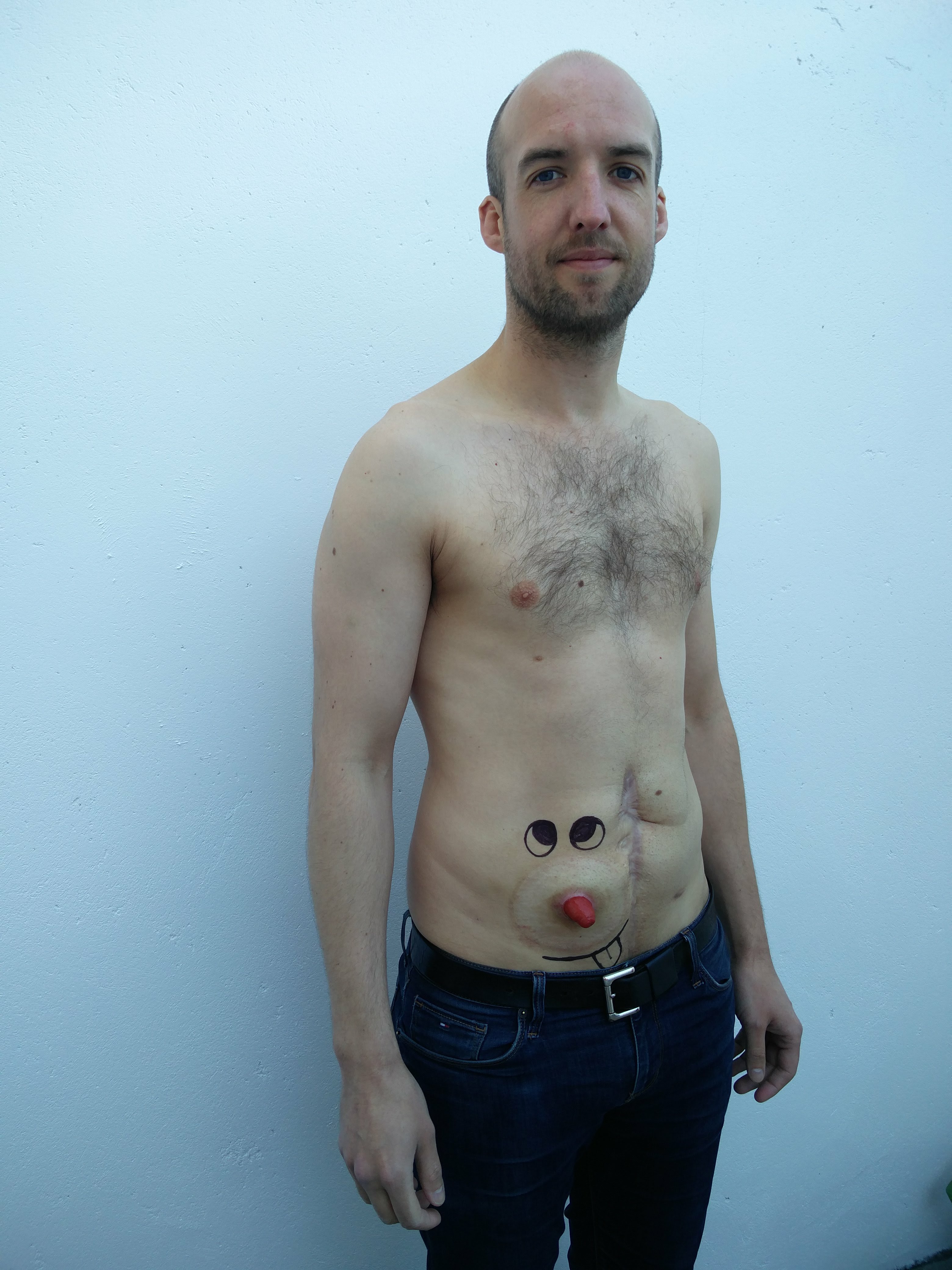
Several people have asked me since the reversal surgery, ‘do you miss it?’
Miss what? Pooing into a bag? Having part of my guts sticking out of me? Not using my bum for nearly a year?
No. I don’t miss any of those things. But it wasn’t bad either. It was an oddly minor thing. I lived with it, then it ended. I suppose that’s how I have felt about much of this weird cancer experience: nothing. And that lack of feeling brings me back round to the foundation of this story – wondering what it all means.
When I first wrote about my misfortune I said ‘my only failure in this whole adventure would be not to learn from it’. Surviving what you might call a near-death experience with little more than scars should be the greatest lift anyone could hope for on their personal development journey. So what have I learned? How have I grown?
Not much.
Sorry.
Even writing this piece has taken a lot of effort, when I normally can’t stop myself from penning adventures. I couldn’t be bothered. I wanted to get on with other stuff, not linger in this disease thing that was handed to me by bad luck.
And in the quiet moments, when I have reflected on what happened, I have rummaged around for a message amongst all the madness and come back up empty-handed. This fruitless search frustrated me for a while. But recently I think I have finally realised that there is meaning in the lack of meaning. I now know what this incident taught me: that I didn’t need it.
I didn’t need cancer to teach me that life is better if you let yourself have fun. Being positive and joyous through the banality of everyday life was not just a tool that I could deploy for surviving difficult times like illness, it was already an achievement in itself. I had already grown, and started this journey from a place that many people have yet to reach. They need the horror of a tumour up their arse to permit themselves to go there. And once they do, I guess they never return, because why would you?
So maybe I did learn something: that I had already qualified for this particular module at the University of Life. I would have skipped it if I had been given the choice. Yet I’m glad I sat through it. I passed the test and now I get to wave my certificate as proof that I know something you might not. I get to tell you about it. And if you happen to be someone who is staring into the abyss right now, grabbing your breath before your own dive into the mire of sickness or uncertainty… who knows, maybe you can take some strength from my experience.
That’s why I wrote this. Not because I thought it was interesting or fun. I wrote it for you. It’s the last thing I need to do before I can put this whole stupid incident behind me. So here you go. Good luck.


Golly. You are so full of humour of life. I met you so many years ago when you were a teenager and now I am 61 and you are a family man in your 30s. I haven’t seen your dad in ages. Life goes on with its busyness. Glad you are well and recovered. Thank you for sharing. You don’t see yourself that you are an inspiration. A message of hope. A sharing of love for life. Enjoy and thank you. Anthea x
Ben and Tony….. Fuckin hero x
Thank you Ben,
For going through all this and sharing with us. I didn’t skip to the end, but I didn’t read everything either. Couldn’t watch your Will video, and don’t care to know who Tony is.
Fuck Tony!!
Congratulations on not only surviving this long ordeal, but also for having Maeve by your side for the journey!!